Introduction
The relentless march of chronic pain can shadow each step. In the sea of lingering pains and aches, sciatica and lupus are two culprits that cause considerable distress.
Sciatica may radiate down one terrain – the sciatic nerve – while lupus goes all out on several bodily fronts. But they may combine in an invasive overlap – a Venn diagram of discomfort.
We’ll explore their cohabitation – unraveling the symptoms that twin under one banner. With insight, the burden may plot a course toward symptom mastery and pursue the most effective treatments, thereby curing a lifelessness marked by pain.
What is Sciatica?
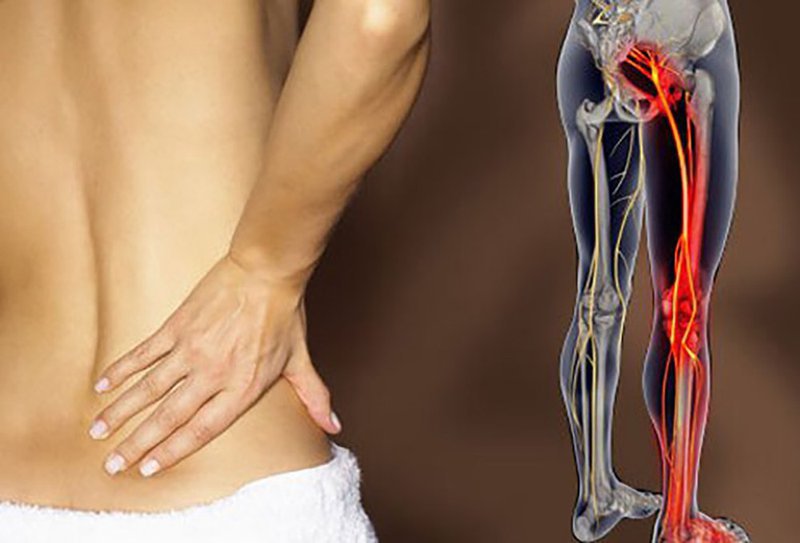
Sciatica is pain which emanates down the sciatic nerve, which runs out of the lower back down the hips, buttocks and down each leg from the back to the buttocks and hips. It may be a result of compression or irritation of the sciatic nerve, typically out of a herniated disc, bone spur, or spinal stenosis. The pain might be moderate to severe and include numbness, tingling, or weakness in the afflicted leg.
What is Lupus?
Lupus (systemic lupus erythematosus, SLE) is an autoimmune condition which commonly impacts the joints, heart, kidneys, skin, and lungs. This happens when the immune system attacks healthy organs and tissues. Lupus signs and symptoms consist of exhaustion, joint pain, pimples, fever and swelling. The progression and severity of lupus varies considerably for every person.
Overlapping Symptoms
Whereas sciatica and lupus affect different body parts, there are some overlapped symptoms. Both conditions could be uncomfortable and painful and it’s hard to tell them apart. For example, lupus sufferers may have sciatica – like joint pain from joint inflammation. Similarly, sciatica causes muscle and joint pain that mimics lupus symptoms.
The Impact of Lupus on Sciatica
Sometimes lupus causes or worsens sciatica. The lupus – induced inflammation can cause swelling in the tissues surrounding the sciatic nerve, increasing the risk of compression and irritation. Additionally, lupus-associated joint pain and stiffness could impact movement and posture of the back, leading to spine anomalies which promote sciatic nerve impingement.
Managing Sciatica and Lupus Together
When dealing with sciatica and lupus, adopting a comprehensive approach to manage symptoms effectively is crucial. Here are some strategies that can help:
1. Medical Treatment:
Consult with healthcare professionals who specialize in treating both sciatica and lupus. They can prescribe appropriate medications to alleviate pain and inflammation, such as nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, and immuno suppressants.
2. Physical Therapy:
Engaging in targeted exercises and stretching routines can help strengthen the muscles surrounding the sciatic nerve, improve flexibility, and reduce pain. Physical therapists can guide individuals through customized programs based on their needs and limitations.
3. Heat and Cold Therapy:
Applying heat or ice packs to the affected area can temporarily relieve pain and inflammation. Alternate between hot and cold treatments to find which works best for you.
4. Lifestyle Modifications:
Adopting a healthy lifestyle can positively impact both sciatica and lupus. Maintain a balanced diet, engage in regular exercise, get sufficient rest, and manage stress levels to support overall well-being.
5.Pain Management Techniques:
Explore alternative therapies such as acupuncture, chiropractic care, and massage therapy to complement conventional treatments. These approaches can help alleviate pain, reduce muscle tension, and promote relaxation.
Differentiating Between Sciatica and Lupus Symptoms
The treatment and diagnosis of sciatica and lupus signs and symptoms should be made clear to differentiate between them. There may be overlapping symptoms, but some characteristics that distinguish the two.
Sciatica is primarily pain that radiates along the sciatic nerve path. The pain can be referred to as sharp, shooting from the lower back or buttock down the leg. It may get worse with movement, prolonged sitting, or certain activities such as lifting heavy objects. Together with the pain, individuals with sciatica might see numbness, tingling or weakness in the affected leg.
However, lupus symptoms can be widespread and affect many body systems. They might suffer fatigue, skin rashes, joint pain, fever and swelling. The joint pain associated with lupus may resemble sciatica but is usually at multiple joints and is accompanied by swelling and redness. Lupus might also create a butterfly rash on nose and cheeks, extreme sensitivity to sunlight, chest discomfort, shortness of breath and kidney damage.
Whereas sciatica is normally present in the lower back, leg and buttock, lupus signs and symptoms are able to occur all through the body. Talk to doctors who could assess your medical history, physical exam and perhaps diagnostic testing to arrive at a proper diagnosis.
- Neurovit Forte: A Comprehensive Guide for Nerve Pain Relief
- Cystic Fibrosis Homeopathic Treatment
- Benefits of Scent Leaf: Unleashing the Health Wonders of this Powerful Herb
- How to Get Health Insurance in Nigeria: A Comprehensive Guide
- Health Benefits of Bitter Leaf: The Ultimate Guide to this Powerful Herb
Treatment Approaches for Sciatica and Lupus
The treatment approaches for sciatica and lupus differ based on the underlying causes and symptoms. Here are some common treatment modalities for each condition:
Treating Sciatica:
1. Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help reduce pain and inflammation associated with sciatica. In more severe cases, oral corticosteroids or muscle relaxants may be prescribed.
2. Physical Therapy: A physical therapist can design a customized exercise program to strengthen the core muscles, improve flexibility, and relieve pressure on the sciatic nerve. They may also incorporate techniques such as manual therapy, traction, or ultrasound for pain relief.
3. Epidural Steroid Injections: An epidural steroid injection may be recommended in cases of persistent or severe pain. It involves injecting a corticosteroid medication directly into the space around the spinal nerve roots to reduce inflammation and alleviate symptoms.
4. Surgical Intervention: If conservative treatments fail to provide relief, surgery may be considered for severe cases of sciatica. Procedures such as discectomy (removal of a herniated disc) or laminectomy (removal of part of the vertebra to relieve pressure) may be performed.
Treating Lupus:
1. Medications:
Lupus treatment often involves a combination of medications to control inflammation, reduce symptoms, and prevent disease flares. These may include nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, antimalarial drugs, immunosuppressants, and biologics.
2. Lifestyle Modifications:
Managing lupus involves adopting a healthy lifestyle. This includes getting regular exercise, maintaining a balanced diet rich in fruits, vegetables, and whole grains, avoiding excessive sun exposure, getting adequate rest, and managing stress levels.
3. Symptom-Specific Treatments:
Additional treatments may be recommended depending on the specific symptoms experienced. For example, skin rashes may be treated with topical creams or antimalarial medications, while kidney involvement may require medications to protect kidney function.
4. Regular Medical Check-up:
Since lupus is a chronic condition, regular medical check-ups are essential. These appointments allow healthcare professionals to monitor disease activity, adjust medications as needed, and address emerging concerns or complications.
It’s important to note that the treatment plans for both sciatica and lupus are highly individualized. Healthcare professionals will consider various factors, including the severity of symptoms, overall health, and the presence of any other medical conditions when developing a personalized treatment approach.
Conclusion
Sciatica and lupus are two different diseases that sometimes share symptoms. Whereas sciatica affects the back and legs via compression of the sciatic nerve, lupus is an autoimmune condition which leads to widespread inflammation throughout multiple body systems. Knowing the characteristics of each condition and looking for proper medical treatment might help individuals deal with their symptoms and enhance quality of life.
Reminder: in case you suspect you have lupus or sciatica, see an expert for a diagnosis and treatment suggestions. They will show you the way to control your condition and ease symptoms.
Frequently Asked Questions (FAQs)
Q1: Can sciatica be a symptom of lupus?
A1: While sciatica is not directly caused by lupus, the inflammation associated with lupus can contribute to sciatic nerve compression, leading to sciatica-like symptoms.
Q2: Is sciatica a permanent condition?
A2: In most cases, sciatica is a temporary condition that improves with time and appropriate treatment. However, in some instances, chronic sciatica may persist and require ongoing management.
Q3: Are there specific risk factors for developing lupus-related sciatica?
A3: The development of sciatica in individuals with lupus can be influenced by factors such as overall disease activity, joint inflammation, and the impact on spinal alignment and mobility.
Q4: Can lifestyle changes help manage sciatica and lupus symptoms?
A4: Yes, adopting a healthy lifestyle, including regular exercise, a balanced diet, stress management, and sufficient rest, can contribute to overall symptom management for both sciatica and lupus.
Q5: Can sciatica and lupus be cured completely?
A5: While there is currently no known cure for either condition, appropriate treatment and self-care measures can help manage symptoms and improve the overall quality of life.
Please note that the above FAQs are created for this article and should not substitute professional medical advice. Consult with healthcare professionals for accurate diagnosis and personalized recommendations.